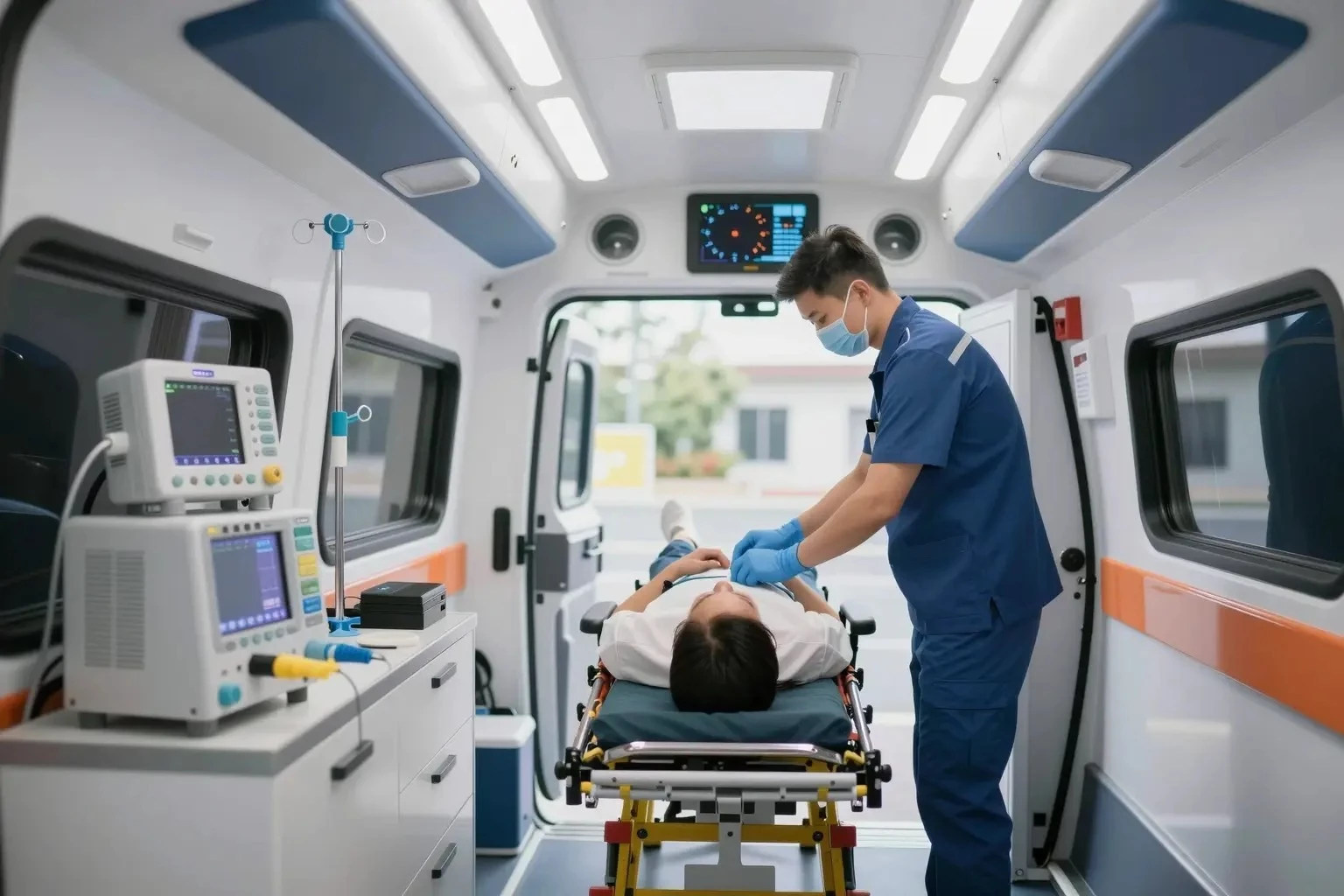
Critical care transport involves the emergency services of transferring patients needing intensive care and life support from one location to another, ensuring stabilization and specialized care during patient transfer.
Definition and Importance
Critical care transport refers to the specialized medical transport of patients requiring intensive care and life support during transit. This service is vital in ensuring that critically ill patients receive continuous medical attention while being moved between healthcare facilities or from the scene of an emergency to a hospital. The importance of critical care transport lies in its ability to bridge the gap between emergency care and definitive treatment, often determining patient outcomes. With state-of-the-art medical equipment and highly skilled paramedics and critical care teams, these transports provide essential stabilization and pre-hospital care. By following established transport protocols, they ensure the safe and efficient interfacility transfer of patients, especially when rapid response and specialized care are needed promptly. Critical care transport is an integral component of modern healthcare systems.
Overview of Critical Care Transport
Critical care transport is a comprehensive medical transport service designed to move patients requiring advanced intensive care and life support between locations. This service is essential for ensuring that patients receive continuous specialized care during transit, whether it is a hospital transfer or an emergency service to a medical facility. The process involves highly trained paramedics and a critical care team equipped with sophisticated medical equipment and protocols to provide stabilization and urgent care when needed. Critical care transport can be conducted via ground ambulance or air ambulance, depending on the situation and distance. The primary aim is to deliver pre-hospital care and ensure the safety and wellbeing of the patient throughout the journey. This service plays a crucial role in healthcare systems, facilitating timely and efficient interfacility transfers;
Types of Critical Care Transport
Critical care transport involves ground ambulances and air ambulances, each equipped for interfacility transfers and emergency services, ensuring intensive care and life support during patient transfer.
Ground Ambulance
Ground ambulances are a fundamental component of critical care transport, offering vital medical transport services for patients in need of intensive care during transit. Equipped with advanced medical equipment and capable of providing essential life support, these vehicles are staffed by trained paramedics and critical care teams. Ground ambulances play a crucial role in patient transfer scenarios, including both emergency services and interfacility transfers. They ensure that patients receive continuous stabilization and pre-hospital care while being swiftly transported to healthcare facilities. Adhering to established transport protocols, ground ambulances can navigate urban and rural environments effectively, providing specialized care tailored to each patient’s urgent needs. Their rapid response capabilities make them indispensable in delivering timely medical interventions, ensuring the highest standards of care throughout the journey, and contributing significantly to positive patient outcomes.
Air Ambulance
An essential element of critical care transport, air ambulances provide rapid medical transport for patients requiring intensive care and life support over long distances or in remote areas. These aircraft are equipped with advanced medical equipment and staffed by highly skilled paramedics and a critical care team, ensuring continuous stabilization and specialized care during patient transfer. Air ambulances are crucial for interfacility transfers and emergency services when ground transport is impractical or time-sensitive. They follow stringent transport protocols to ensure safety and efficiency. Capable of reaching inaccessible areas quickly, air ambulances play a vital role in delivering urgent care and enhancing patient outcomes by reducing travel time to hospital facilities. Their ability to provide prompt, comprehensive pre-hospital care is a testament to their indispensable role in modern healthcare systems.
Key Components of Critical Care Transport
Critical care transport relies on medical equipment, life support systems, skilled paramedics, and a dedicated critical care team to ensure effective patient transfer and specialized care.
Medical Equipment and Life Support
In critical care transport, the availability of advanced medical equipment and reliable life support systems is paramount to providing high-quality patient transfer services. These transports are equipped with state-of-the-art devices such as ventilators, defibrillators, and infusion pumps to ensure continuous intensive care. Monitoring equipment, including ECG machines and pulse oximeters, is essential for real-time assessment of a patient’s condition. The integration of portable laboratory equipment allows for quick diagnostic evaluations. These tools are crucial in maintaining patient stabilization and supporting the efforts of the critical care team and paramedics. By adhering to strict transport protocols, the equipment ensures that patients receive the necessary specialized care throughout the journey. The seamless operation of these systems is vital in addressing urgent care needs, ultimately enhancing patient outcomes in medical transport.
Role of Paramedics and Critical Care Team
The paramedics and critical care team are integral to the success of critical care transport, providing expert medical transport and intensive care during patient transfer. These healthcare professionals are trained to operate advanced medical equipment and deliver essential life support services. Their expertise ensures effective stabilization and specialized care tailored to each patient’s needs. Paramedics are adept at making swift clinical decisions, while the critical care team, often including nurses and physicians, brings a comprehensive approach to managing complex cases. Together, they adhere to rigorous transport protocols to provide seamless pre-hospital care. The collaboration within this team is vital for addressing urgent care needs and ensuring a smooth interfacility transfer. Their dedication and skills significantly enhance patient outcomes, making them crucial in emergency services.
Critical Care Transport Protocols
Critical care transport follows stringent transport protocols to ensure effective medical transport, patient stabilization, and specialized care during patient transfer and emergency services.
Transport Protocols and Procedures
In critical care transport, adhering to detailed transport protocols and procedures is essential for ensuring safe and efficient medical transport. These protocols provide a structured approach for the critical care team, guiding them through each stage of the patient transfer process. Key components include pre-transport assessments, ensuring the readiness of medical equipment, and continuous monitoring of the patient’s condition. Protocols also cover communication procedures between paramedics and receiving healthcare facilities, ensuring that all medical data is accurately conveyed. These procedures ensure seamless stabilization, pre-hospital care, and intensive care during transit. By following standardized guidelines, the team can swiftly address urgent care needs and respond to emergencies, thereby enhancing patient safety and outcomes. These protocols are vital for maintaining the high standards expected in emergency services and interfacility transfers.
Stabilization and Pre-Hospital Care
In critical care transport, stabilization and pre-hospital care are vital components for ensuring patient safety during medical transport. These processes begin with an assessment by the paramedics and critical care team, who evaluate the patient’s condition to determine the necessary interventions. Stabilization involves managing vital signs and supporting life functions using advanced medical equipment and life support systems. This phase prepares patients for safe patient transfer by addressing immediate medical needs and preventing deterioration. Pre-hospital care includes continuous monitoring and treatment en route, ensuring seamless care from the point of contact to the receiving facility. The team follows established transport protocols to provide intensive care and urgent care, crucial for enhancing patient outcomes. Effective stabilization and pre-hospital care are essential in bridging the gap between emergency services and hospital-based treatment.
Interfacility and Hospital Transfers
Interfacility transfers involve medical transport between healthcare facilities, ensuring intensive care and life support through skilled critical care teams and efficient transport protocols.
Interfacility Transfer Processes
The interfacility transfer process is a critical component of critical care transport, designed to safely move patients between healthcare facilities while maintaining the highest standards of intensive care. This process begins with thorough coordination between the referring and receiving facilities, ensuring all parties are informed and prepared for the patient transfer. The critical care team, including skilled paramedics, prepares the patient by stabilizing vital signs and ensuring the readiness of medical equipment and life support systems. Throughout the transfer, continuous monitoring and communication are maintained to address urgent care needs. Detailed transport protocols guide the entire process, ensuring patient safety and adherence to medical standards. Upon arrival, a seamless handover to the receiving facility ensures continuity of care. Effective interfacility transfers are essential for optimizing patient outcomes and providing comprehensive pre-hospital care.
Hospital Transfer Coordination
Effective hospital transfer coordination is a cornerstone of successful critical care transport, ensuring seamless patient transfer between medical facilities. This process requires meticulous planning and communication among healthcare providers, the critical care team, and paramedics. Coordination begins with identifying the patient’s medical requirements, confirming the readiness of the receiving facility, and organizing necessary medical equipment and life support systems. Clear communication channels are established to relay patient information and medical status to all involved parties. Transfer coordination also involves scheduling transportation, whether via ground ambulance or air ambulance, based on urgency and distance. Adherence to established transport protocols ensures patient safety and continuity of intensive care during transit. Upon arrival, a structured handover procedure is conducted to maintain the level of specialized care required. This comprehensive coordination is vital for optimizing patient outcomes in interfacility transfers.
Challenges in Critical Care Transport
Critical care transport faces challenges like ensuring rapid response and emergency services, managing specialized care needs, and adhering to strict transport protocols.
Rapid Response and Emergency Services
In critical care transport, rapid response and efficient emergency services are crucial for ensuring timely and effective patient transfer. The ability to respond quickly to emergencies can significantly impact patient outcomes, especially when dealing with life-threatening situations. This requires a well-coordinated system where the critical care team, including paramedics, is always prepared. The deployment of medical transport vehicles such as ground ambulances and air ambulances must be swift and strategically located to cover extensive areas. Advanced medical equipment and life support systems must be readily available to provide immediate intensive care. Additionally, adherence to established transport protocols ensures that all actions are systematic and efficient. Effective communication with hospitals and other healthcare facilities is essential for coordinating specialized care and maintaining continuity of treatment during urgent care scenarios.
Specialized Care and Urgent Care Needs
Addressing specialized care and urgent care needs in critical care transport requires a highly skilled critical care team equipped with advanced medical equipment and life support systems. Each patient’s unique medical requirements must be assessed and managed with precision to ensure optimal outcomes during patient transfer. The team of paramedics and healthcare professionals must be trained to deliver intensive care tailored to conditions such as cardiac emergencies, respiratory failure, or trauma. Transport protocols guide the team in providing continuous monitoring and interventions en route, ensuring effective stabilization. Communication with receiving facilities is crucial for coordinating ongoing specialized care upon arrival. Meeting these needs requires agility, expertise, and seamless integration of pre-hospital care practices, ensuring that patients receive the highest level of care throughout the medical transport process, even in the most demanding situations.
Critical care transport is an essential component of modern healthcare, providing crucial medical transport for patients requiring intensive care and life support. Whether through ground ambulance or air ambulance, these services ensure that patients receive continuous specialized care during patient transfer. The roles of paramedics and the critical care team are vital, with their expertise ensuring effective stabilization and adherence to transport protocols. Addressing urgent care needs and managing interfacility transfers are significant challenges, yet these processes are critical for improving patient outcomes. The integration of advanced medical equipment and rapid emergency services further underscores the importance of this specialized transport. Ultimately, critical care transport represents a lifeline for critically ill patients, bridging the gap between immediate medical attention and comprehensive hospital care, and is indispensable in achieving positive health outcomes.